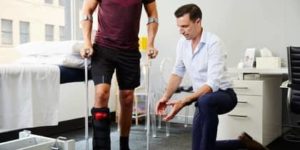
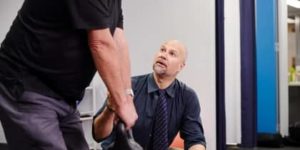
Our Expert Services
Available as usual in the clinic, or via video for your convenience. Click here for more information.
We are a highly skilled team of expert Physiotherapists, catering to the Sydney CBD, Eastern Suburbs, North Shore, Inner West and Northern Beaches. Our passion is ensuring you receive the safest and most-effective health solutions, so whether you're looking for Physiotherapy treatment, Pilates classes or Massage Therapy, our physical therapists are here to help.
Preferred Physiotherapy Provider
Trusted by
Welcome to Sydney's Most-Trusted Physiotherapy Clinics

If you have been looking for physiotherapy treatments in Sydney or surrounding areas, feel free to call us at 02 9252 5770 or send us an email at reception@ssop.com.au.